Message from Program Director
When you train here, you don’t just complete three years of residency — you become the physician you’ve always envisioned.
We like to say we “train where complexity meets community” because that’s exactly what makes our program unique: the challenge of high-acuity medicine combined with the privilege of serving a diverse patient population.
What You’ll Experience
- Hands-On, Always: Every part of your training — including continuity clinic — happens right here on-site with faculty who are dedicated teachers and mentors.
- Critical Thinking Culture: We foster curiosity. You’ll be encouraged to think like a scientist, challenge assumptions, and focus on advancing health equity.
- POCUS in Your Pocket: Ultrasound is not an add-on; it’s integral to daily practice. Every inpatient team has access to point-of-care ultrasound, supported by formal training from nationally recognized faculty.
- Connected Campus: Our close partnership with New York Medical College means endless opportunities for teaching, research, and community engagement.
- Wellness Matters: Wellness isn’t an afterthought here. We integrate initiatives across all five domains of well-being throughout the year, ensuring you feel supported both inside and outside the hospital.
Beyond Training
- Solid foundation in general medicine
- Exposure to diverse subspecialties
- Proven fellowship success nationwide
- Opportunities for research, quality improvement, and high-value care projects
And most importantly — you’ll be part of a community that cares for one another.
Our People
Our residents come from across the U.S. and nine different countries, bringing unique perspectives and experiences. That diversity strengthens our program and fosters a true sense of belonging.
A Message from the Program
Most of all, you’ll find that this is a place where you are supported, challenged, and inspired — not just as a physician, but as a person.
We look forward to welcoming you to our community.
Program Overview
The Internal Medicine Residency Program at Westchester Medical Center has 63 categorical residents. Through collaboration with the WMC Anesthesiology, Neurology and Physical Medicine & Rehabilitation residency programs, 23 additional categorical base year interns train with our program during their first year.
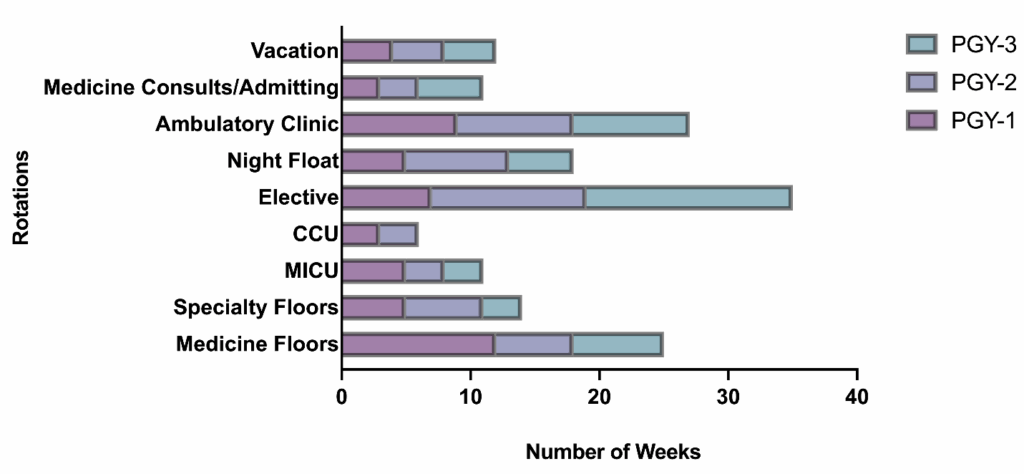
Our program follows a 6 + 2 schedule (six weeks inpatient; two weeks ambulatory). Below is an example of our current annual schedule.
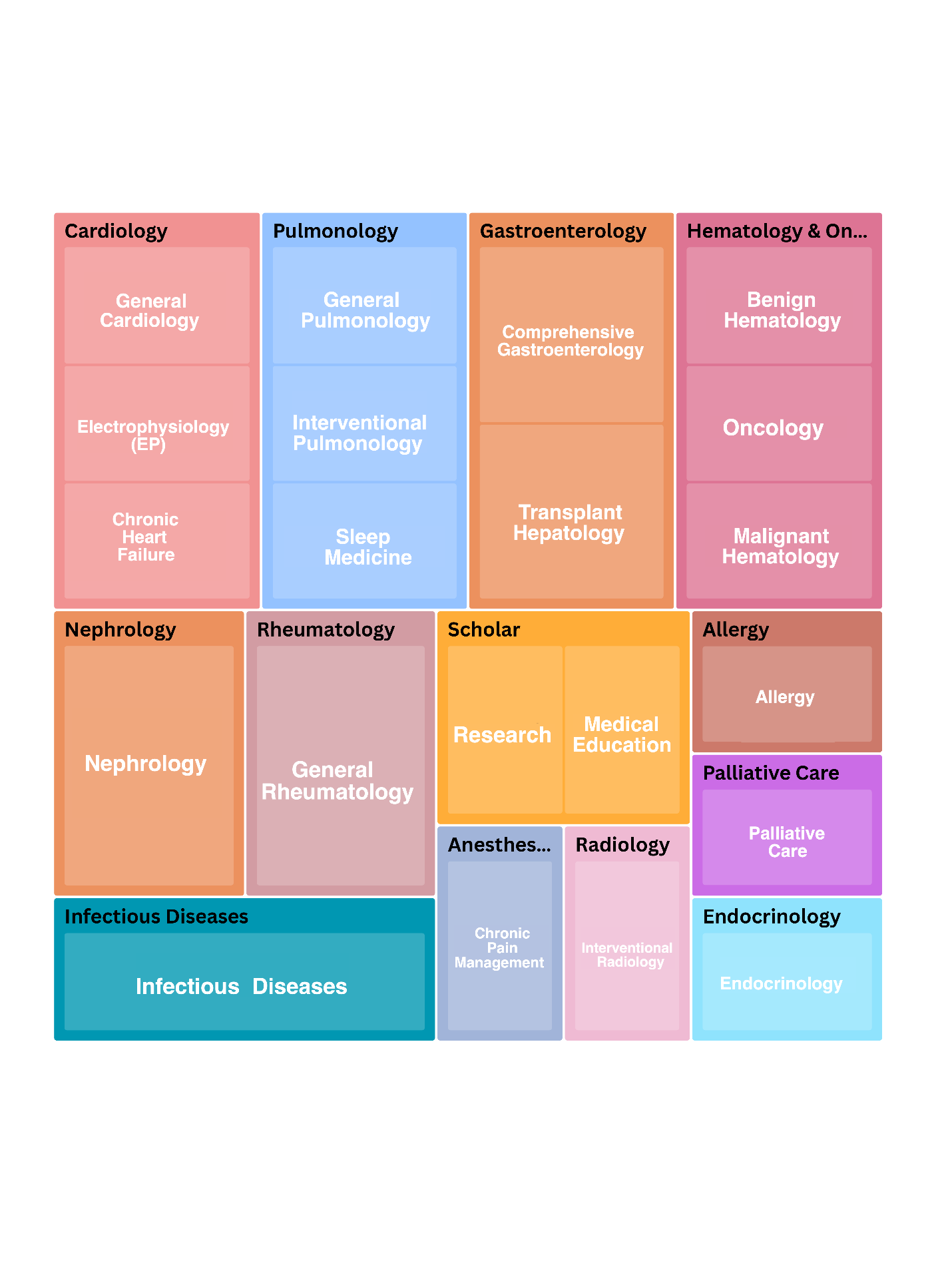
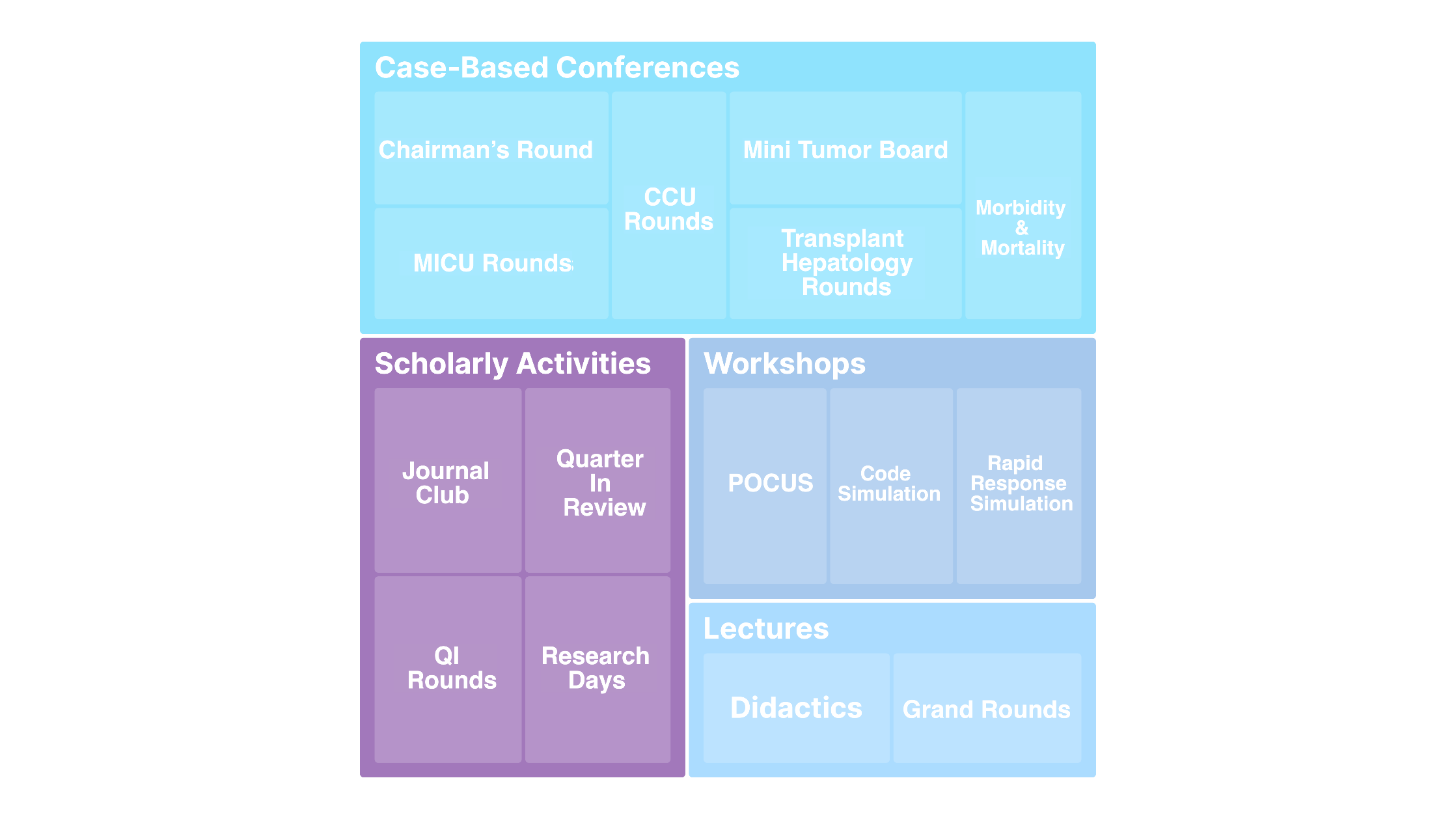
Program Curriculum
How to Apply
Thank you for your interest in the Westchester Medical Center/New York Medical College Internal Medicine Residency Training Program at Westchester Medical Center. Together, they comprise a major academic medical center. Our program is fully accredited by the Accreditation Council for Graduate Medical Education (ACGME).
Criteria for Applicants
Applicants must submit at least three letters of recommendation dated within the current academic year. There is no particular requirement for which type of faculty/supervisors write your letters. We prefer that they are written by faculty who are the most familiar with applicants.
While we prefer candidates not more than five years out of medical school, an applicant involved in a post-graduate clinical environment will be considered.
USMLE or COMLEX Steps 1 and 2 must be passed in order to be considered (step 2 results can be pending at the time of interview but must have a passing score in order to be ranked).
We do not have a firm cut off on USMLE or other exam scores. We review all applicants from a holistic standpoint, considering their overall diversity, skills, and experience.
Interview Schedule & Criteria
We will notify applicants through Thalamus as to whether they have been selected for an interview. Applications should be submitted through the Electronic Residency Application System (ERAS), which can be accessed using at https://apps.aamc.org/myeras. Applications may be submitted starting September 3, 2025, and Internal medicine residency programs may begin reviewing applications in ERAS on September 24, 2025.
Our residency interviews for the 2025-2026 application cycle will be held virtually.
Our program will begin our first round of invitations in early October. Interviews will take place October 20 through December 18. Candidates will be provided with detailed information regarding the logistics of the interview days.
Visa Sponsorship
Passage of USMLE Step 3 is strongly encouraged for all applicants applying from abroad.
Westchester Medical Center will accept individuals on J1 Visas sponsored by the ECGMG/Intealth.
More information about the residency program is available on our Fellowship and Residency Electronic Interactive Database (FREIDA) listing.
Program Signaling
While we preferentially review applications from those who signal our program, we also consider applicants who do not signal us.
Frequently Asked Questions
Contact Us
Austin Charnis
Residency Program Manager, Internal Medicine
[email protected]
Austin Charnis, a native of Westchester County, has been the administrator of the Internal Medicine Residency Program at Westchester Medical Center since 2019. Prior to this role Austin held positions at our institution as fellowship coordinator in medicine subspecialties and administrative assistant in the Office of Graduate Medical Education. His professional interests include medical education, communications and technology, and he is highly passionate about supporting our residents, faculty and staff.
Current Residents
-
Assem Al Refaei – University of Jordan Faculty of Medicine
-
Fatima Arslan – Aga Khan University Medical College
-
Jovan Bertrand – Hackensack Meridian School of Medicine
-
Kira Burdman – Des Moines University College of Osteopathic Medicine
-
Anthony Capasso – Ross University School of Medicine
-
Zainab Chaudhry – Ameer-ud-Din Medical College
-
Sunit Chhetri – B.P. Koirala Institute of Health Sciences
-
James Glenn – Touro College of Osteopathic Medicine
-
Omar Gobji – New York Medical College
-
Gina Grass – New York Medical College
-
Hoore Jannat – Khyber Medical College
-
Omkar Jha – Kathmandu University School of Medical Sciences
-
Kashish Magnani – Surat Municipal Institute of Medical Education and Research
-
Srista Manandhar – B.P. Koirala Institute of Health Sciences
-
Rangsheng Mei – Wenzhou Medical College
-
Oghenemega Okoloko – New York Medical College
-
Harsha Pattnaik – Lady Hardinge Medical College
-
Sreejan Saha – New York Institute of Technology College of Osteopathic Medicine
-
Bahaa Salama – University of Alexandria Faculty of Medicine
-
Kriti Shah – Northwestern University Feinberg School of Medicine
-
Manisha Verma – Central Michigan University College of Medicine
- Rimsha Ahmad, MBBS – Aga Khan University Medical College
- Daniel Basta, MD- Hackensack Meridian School of Medicine
- Maxwell Charlat, MD – SUNY Upstate Medical University Alan and Marlene Norton College of Medicine
- Ashley Covatto, DO – Touro College of Osteopathic Medicine
- Sara Elattar, MBBCh – University of Alexandria Faculty of Medicine
- Kristjana Frangaj, MD – Oakland University William Beaumont School of Medicine
- Christopher Fu, DO – Touro College of Osteopathic Medicine
- Heng Jiang, MD – University of Nebraska College of Medicine
- Amit Krishnan, MD – New York Medical College
- Victoria Maksymiuk, MD – New York Medical College
- Christopher Poletes, MBBCh – Royal College of Surgeons in Ireland School of Medicine
- Sarah Rahni, DO – Touro College of Osteopathic Medicine
- Nabel Rajab Basha, MBBS – Alfaisal University College of Medicine
- Miranda Ribner, MD – Cooper Medical School of Rowan University
- Rohan Sampat, MD – Hofstra Northwell School of Medicine
- Eric Schwender, MBBCh – Royal College of Surgeons in Ireland School of Medicine
- Christine Seaton, MD – Albert Einstein College of Medicine of Yeshiva University
- Wayne Seaton, MD – Albert Einstein College of Medicine of Yeshiva University
- Shota Someya, MBBS, PhD – University of New South Wales Faculty of Medicine
- Alyssa Wruble, MD – Albert Einstein College of Medicine of Yeshiva University
- Zhang Hall, MD – SUNY Downstate Medical Center College of Medicine
- Fatima Arslan, MD – Aga Khan University Medical College
- Jessica Accardi, MD – University of South Carolina School of Medicine Greenville
- Curie Ahn, MD – Tufts University School of Medicine
- Sanjana Arsha, MD – New York Medical College
- Steven Buffer, MD – Hackensack Meridian School of Medicine
- Lauren Coritt, MD – University of Vermont Larner College of Medicine
- Muhammad Furqan, MBBCh – Trinity College Dublin School of Medicine
- Jeff Gao, MD – Rutgers New Jersey Medical School
- Jasmine Garg, MD – New York Medical College
- Yosef Hassid, MD – New York Medical College
- Syed Sadam Hussain, MBBS – Khyber Medical College
- John Kangarlu, MD – SUNY Upstate Medical University College of Medicine
- Dovid Kotkes, MD – Frank H. Netter MD School of Medicine at Quinnipiac University
- Avraham Marcucci, DO – Touro College of Osteopathic Medicine
- Eshaan Parikh, MD – Cooper Medical School of Rowan University
- Elona Poltiyelova, DO – New York Institute of Technology College of Osteopathic Medicine
- Bilal Rehman, MD – University of Oklahoma College of Medicine
- Dafna Somogyi, MD – New York Medical College
- Moshe Spira, MD – Albert Einstein College of Medicine of Yeshiva University
- Rehan Tariq, MD – Oakland University William Beaumont School of Medicine
- Rachel Topp, MD – New York Medical College
- Ashish Tripathi, MBBS – Government Medical College Amritsar
- Amha Weldehana, MD – Addis Ababa University Faculty of Medicine
Ryan Cheikhali, MD – Morehouse School of Medicine
Jesse Silverman, MD – New York Medical College
Wei Tang, MD – Zhejiang University School of Medicine
Program Alumni
- Cory Benjamin – Hematology/Oncology, Westchester Medical Center, Valhalla, NY
- Dennis Boyle – Pulmonary/Critical Care, Westchester Medical Center, Valhalla, NY
- Tzvi Fishkin – Cardiovascular Disease, Nassau University Medical Center, East Meadow, NY
- Gabriel Heering – Gastroenterology, Westchester Medical Center, Valhalla, NY
- Aatif Khurshid – Hematology/Oncology, Westchester Medical Center, Valhalla, NY
- Dana Krinsky – Endocrinology, Icahn School of Medicine at Mount Sinai, New York, NY
- Matthew Mcmaster – Cardiovascular Disease, Nuvance Health at Danbury Hospital, Danbury CT
- Demetrios Papademetriou – Infectious Disease, University of California, San Diego, CA
- Sreshta Paranji – Hematology/Oncology, Renaissance School of Medicine at Stoney Brook, Stoney Brook, NY
- Vihanga Perera – Rheumatology, Geisinger Health, Danville, PA
- Matthew Seplowe – Cardiovascular Disease, Staten Island University Hospital, Staten Island, NY
- Pritika Sharma – Hematology/Oncology, Westchester Medical Center, Valhalla, NY
- Fatima Aguilar – Nephrology, Montefiore Medical Center, Bronx NY
- Yaagya Ahlawat – Hematology/Oncology, Westchester Medical Center, Valhalla, NY
- Basha Behrman – Cardiovascular Disease, Houston Methodist Hospital, Houston, TX
- Shoma Bommena – Gastroenterrology, University of Arizona, Tuscon, Arizona
- Dennis Boyle – Infectious Disease University of South Florida, Tampa FL
- Raja Chakinala – Gastroenterology, Guthrie, Sayre PA
- Mekeda Dawkins – Gastroenterology, Westchester Medical Center, Valhalla, NY
- Michael Dolan – Infectious Diesease, Montefiore Medical Center, Bronx, NY
- Andre Esteves – Pulmonary/Critical Care, Memorial Sloan Kettering Cancer Center, New York, NY
- Rohan Kapur – Hematology/Oncology, Maimonides Medical Center, Brooklyn, NY
- Menasche Krupka – Gastroenterology, Westchester Medical Center, Valhalla, NY
- Juliet Meir – Hematology/Oncology, Zucker School of Med / LIJ at North Shore University, Manhasset, NY
- Kelsey McManus – Infectious Diseases, Westchester Medical Center, Valhalla, NY
- Jay Patel – Cardiovascular Disease, Westchester Medical Center, Valhalla, NY
- Nirali Sanghavi – Rheumatology, Westchester Medical Center, Valhalla, NY
- Sarah Subhan – Rheumatology, University of South Carolina/Prisma Health, Columbia, SC
- Andy Wang – Cardiology, Deborah Heart and Lung Center, Browns Mills, NJ
- Alex Weber – Hematology/Oncology, Westchester Medical Center, Valhalla, NY
- Michael Yam – Endocrinology, University of Wisconsin, Madison, WI
- Allen Zeng, Endocrinology, Westchester Medical Center, Valhalla, NY
- Lillian Chang – Rheumatology, Geisinger School of Medicine, Scranton, PA
- Sungsoo Kim – Nephrology, Icahn at Mount Sinai, New York, NY
- Levy Jo Manuntag – Palliative Medicine, MD Anderson Cancer Center, Houston TX
- Liana Michaud – Cardiology, Westchester Medical Center, Valhalla, NY
- Alexander Ogilvy – Infectious Diseases, George Washington University, Washington, DC
- Areen Pitaktong – Pulmonology, Westchester Medical Center, Valhalla, NY
- Joseph Quintas – Hematology/Oncology, Westchester Medical Center, Valhalla, NY
- Aaron Schluger – Gastroenterology, Westchester Medical Center, Valhalla, NY
- Avisha Shah, MD – Cardiology, Westchester Medical Center, Valhalla, NY
- Shantanu Solanki – Gastroenterology, MD Andereson Cancer Center, Houston, TX
Allergy and Immunology
- Rutgers-New Jersey Medical School
Cardiology-Cardiovascular Disease
- Brown University
- Mount Sinai Beth Israel
- Montefiore/Albert Einstein Hospital
- University of Miami Health System
- Maimonides Hospital
- Methodist Hospital
- Lehigh Valley Health Network
- Loma Linda University
- Montefiore Hospital
- Newark Beth Israel Medical Center
- Tulane University x2
- University of Oklahoma
- University of Texas at Houston
- Westchester Medical Center x5
Cardiology-Interventional
- Columbia University
Cardiology-Research
- Kansas Medical Center
Cardiology-Structural Interventions
- Houston Methodist Hospital
Clinical Nutrition
- Cleveland Clinic
Endocrinology, Diabetes and Metabolism
- Einstein College of Medicine / Montefiore Medical Center
- Dartmouth Hitchcock Medical Center
- University of Alabama at Birmingham
Gastroenterology
- Henry Ford Health
- Oakland University William Beaumont
- University of Connecticut x2
- University of Iowa
- Westchester Medical Center x5
Gastroenterology-Advanced Endoscopy
- Stony Brook University Hospital
Heal Initiative
- University of California-SF
Hematology & Medical Oncology
- Baylor College of Medicine
- North Shore University / Long Island Jewish Medical Center
- SUNY Downstate Medical Center
- University of Vermont
- Westchester Medical Center x3
Infectious Diseases
- Northwell Health
- Westchester Medical Center
Medical Education
- Boston University
Nephrology
- Baylor College of Medicine
- Beth Israel Deaconess Hospital
- Icahn School of Medicine @ Mount Sinai
- Massachusetts General Hospital
- New York University
- University of Washington-Seattle
- Westchester Medical Center x4
Pulmonary & Critical Care Medicine
- Albany Medical College
- Mayo Clinic-AZ
- New York Presbyterian Hospital-Queens
- Spectrum Health @ Michigan State University
- Saint Louis University
- Westchester Medical Center x4
Rheumatology
- Loma Linda University
- University of Connecticut
- University of Southern California
- Washington University in St. Louis
- Westchester Medical Center x3
Our Clinical Locations
Westchester Medical Center
Westchester Medical Center shares its leafy campus with New York Medical College in Valhalla, NY, approximately 20 miles north of New York City. It is a Level 1 Trauma and Burn Center and a major hub for specialized care referrals. Here, we take care of patients from a very large catchment area stretching from the northern border of New York City to the Catskill Mountains.
WMC has a pediatric hospital (Maria Fareri Children’s Hospital) with eight dedicated pediatric operating rooms as well as many other non-operating room anesthetizing sites, including MRI, radiation and nuclear medicine, and endoscopy. The Ambulatory Care Pavilion, which opened in July 2019, added many anesthetizing locations, both OR and Non-OR.
Construction is underway on the 128-bed state-of-the-art WMC Critical Care Tower, a $220 million project that when completed will span 162,000 square feet over five floors. Our caseload includes a full profile of cardiac, interventional pulmonary and thoracic, complex orthopedic, neurosurgical and solid organ transplant interventions, to name the busiest services. We have a large heart failure and ECMO referral program. Trauma orthopedics and surgery provide our residents a great variety of “open” cases. Residents participate in minimally invasive and robotic interventions in gynecologic-oncology, urology, colorectal, endocrine and thoracic surgery, as well as complex cardiac and neurological endovascular interventions, both pediatric and adult. The Acute and Chronic Pain Management care rotations cover both the pediatric and adult inpatients and outpatients, including complex consultations for patients in the Burn ICU.